Anesthesiologists Manual of Surgical Procedures is a comprehensive guide, detailing anesthetic techniques for optimal perioperative patient management, covering diverse surgical specialties․
This resource provides essential knowledge for successful anesthetic care, navigating the complexities of procedures before, during, and after surgery․
Purpose and Scope of the Manual
This manual serves as a top-to-bottom guide for anesthesiologists, focusing on effective perioperative management․ Its primary purpose is to maximize the benefit-risk ratio when providing neuraxial analgesia and other anesthetic techniques․
The scope encompasses a broad range of surgical procedures, including neurosurgery, obstetrics, pediatrics, orthopedics, and cardiac/thoracic cases․ It details anesthetic adaptations for minimally invasive procedures, alongside comprehensive pharmacological information and complication management strategies․
Furthermore, the manual supports establishing acute pain services and fostering interdepartmental collaboration, ensuring optimal patient outcomes throughout the surgical journey․
Historical Development of Perioperative Anesthesia
Early anesthesia relied on rudimentary methods, evolving from etherization in the mid-19th century to the introduction of chloroform and subsequent advancements in inhalation agents․ The field progressed with the development of neuromuscular blocking agents and improved monitoring technologies․
Over time, regional anesthesia techniques gained prominence, offering targeted pain control with reduced systemic effects․ Contemporary anesthesia incorporates multimodal analgesia, personalized approaches, and increasingly, artificial intelligence․
This manual builds upon this rich history, providing modern techniques grounded in decades of research and clinical experience, ensuring patient safety and comfort․
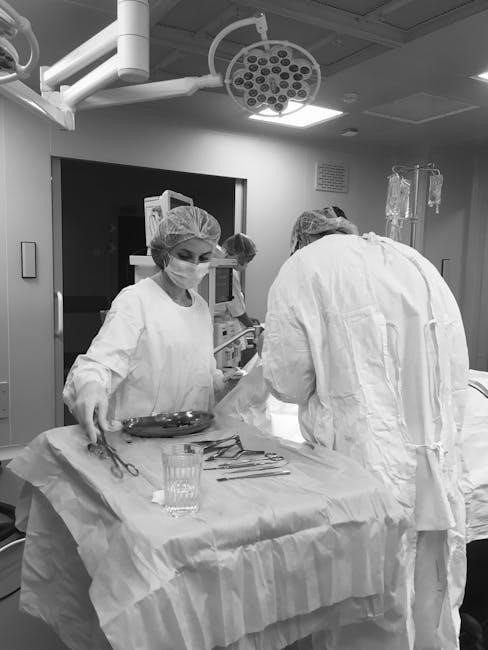
Preoperative Assessment & Planning
Thorough patient evaluation and risk stratification are crucial for developing individualized anesthesia plans tailored to specific surgical procedures, maximizing safety and efficacy․
Patient Evaluation and Risk Stratification
Comprehensive preoperative assessment is paramount, encompassing a detailed medical history, physical examination, and review of existing conditions․ Identifying potential risks – cardiac, pulmonary, or other comorbidities – guides anesthetic planning․
Risk stratification utilizes scoring systems and clinical judgment to predict postoperative complications․ This process informs decisions regarding monitoring, medication protocols, and contingency planning․ Accurate evaluation ensures tailored anesthesia, optimizing patient safety throughout the surgical journey and minimizing adverse events․
Preoperative Medication Protocols
Establishing standardized protocols for preoperative medications is crucial for optimizing patient outcomes․ These protocols may include anxiolytics to reduce anxiety, antiemetics to prevent nausea, and medications to manage specific conditions like hypertension or arrhythmias․
Careful consideration of drug interactions and patient allergies is essential․ Protocols should be tailored to the individual patient and the planned surgical procedure, aiming to minimize side effects and enhance the anesthetic experience․
Development of Anesthesia Plans Based on Surgical Procedure
Anesthesia plans must be individualized, meticulously aligned with the specifics of each surgical procedure․ Factors like surgical duration, anticipated blood loss, patient positioning, and potential for hemodynamic instability all dictate anesthetic choices․
Neurosurgical procedures demand precise cerebral perfusion management, while cardiac surgeries necessitate careful hemodynamic control․ Regional anesthesia may be suitable for orthopedic cases, minimizing systemic effects․ Thorough surgical consultation is paramount for optimal planning․
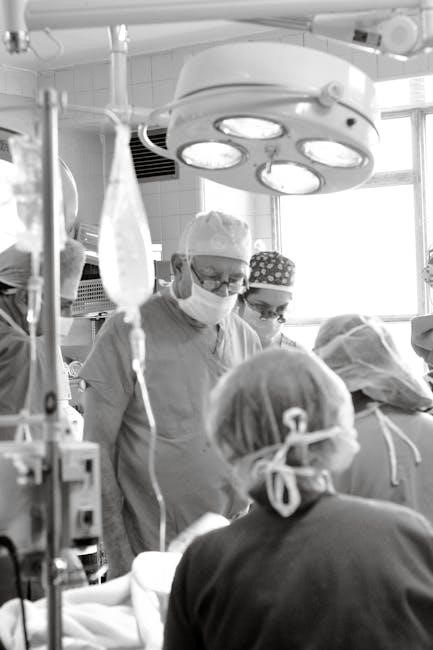
Airway Management in Surgical Procedures
Securing a patent airway is fundamental, utilizing techniques like endotracheal intubation, with careful tube selection and confirmation for optimal ventilation during surgery․
Techniques for Securing the Airway
Establishing a secure airway is paramount in surgical anesthesia, employing diverse techniques tailored to individual patient anatomy and clinical scenarios․ These include direct laryngoscopy, utilizing a Macintosh or Miller blade for visualization of the vocal cords, and indirect laryngoscopy with video assistance․
Furthermore, supraglottic airway devices, such as laryngeal masks and i-gels, offer alternatives for simpler airway management․ Fiberoptic intubation proves invaluable in challenging cases, while cricothyrotomy serves as a last resort for failed intubation; Proper preparation, including preoxygenation and positioning, significantly enhances success rates․
Management of Difficult Airway Scenarios
Difficult airway management demands a systematic approach, prioritizing patient safety and employing contingency plans․ The LEMON assessment – Look Externally, Evaluate the 3-3-2 rule, Mallampati score, Obstruction, and Neck mobility – aids in predicting challenges․
Strategies include utilizing alternative airway devices, awake intubation with fiberoptic bronchoscopy, and surgical airway establishment․ Maintaining oxygenation with bag-valve-mask ventilation or transtracheal jet ventilation is crucial․ Experienced assistance and a calm, methodical approach are essential for successful resolution․
Endotracheal Tube Selection and Confirmation
Endotracheal tube (ETT) selection considers patient size, age, and the surgical procedure․ Appropriate cuff volume is vital for a secure seal․ Confirmation of correct placement is paramount, utilizing multiple methods․
Auscultation of bilateral breath sounds, end-tidal carbon dioxide (ETCO2) detection, and chest X-ray verification are standard practices․ Fiberoptic bronchoscopy offers direct visualization․ Vigilant monitoring for esophageal intubation is crucial, alongside continuous assessment of tube position throughout the surgical procedure․
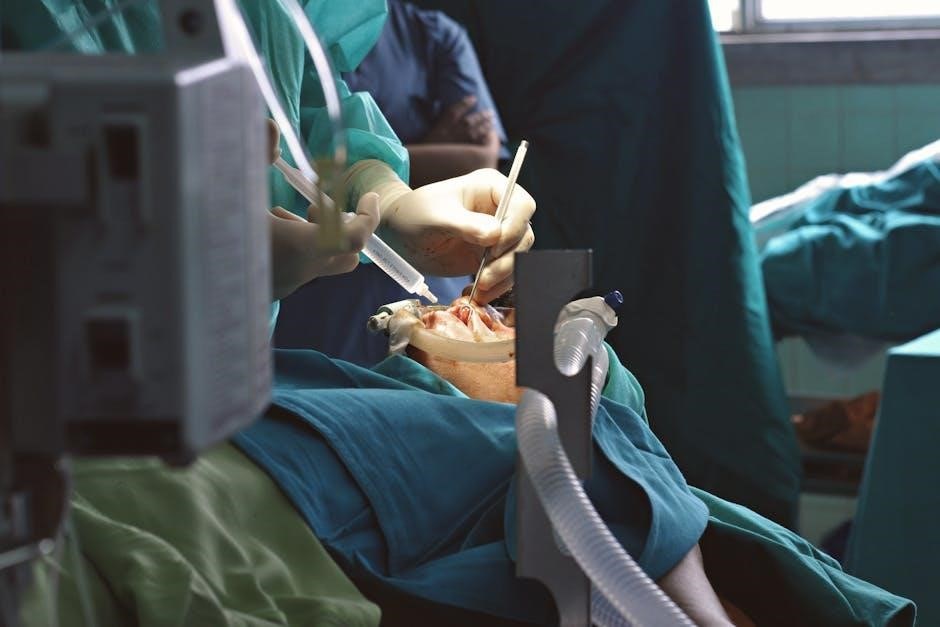
Cardiovascular Considerations
Cardiovascular stability during surgery requires meticulous hemodynamic monitoring and prompt intervention for hypotension or hypertension, utilizing pharmacological agents as needed․
Hemodynamic Monitoring During Surgery
Effective hemodynamic monitoring is crucial for guiding fluid management and optimizing cardiac output throughout surgical procedures․ Anesthesiologists Manual of Surgical Procedures emphasizes utilizing a combination of non-invasive and invasive techniques․
These include continuous arterial blood pressure, central venous pressure (CVP), pulse oximetry, and electrocardiography (ECG)․ More advanced monitoring, such as pulmonary artery catheters (PAC) or transesophageal echocardiography (TEE), may be indicated based on patient comorbidities and surgical complexity․
Careful interpretation of these parameters allows for early detection and correction of hemodynamic instability, ensuring patient safety and optimal surgical outcomes․
Management of Hypotension and Hypertension
Hypotension and hypertension require prompt and tailored interventions during surgery, as detailed in Anesthesiologists Manual of Surgical Procedures․ Hypotension management involves fluid resuscitation, vasopressors (e․g․, phenylephrine, norepinephrine), and addressing underlying causes like hypovolemia or anesthetic-induced vasodilation․
Hypertension necessitates identifying reversible factors – pain, surgical stimulation, or inadequate analgesia․ Treatment options include deepening anesthesia, antihypertensive agents (e․g․, beta-blockers, calcium channel blockers), and careful titration to maintain cerebral perfusion․
Continuous hemodynamic monitoring guides these interventions․
Pharmacological Interventions for Cardiac Stability
Maintaining cardiac stability relies on strategic pharmacological interventions, as outlined in Anesthesiologists Manual of Surgical Procedures․ For bradycardia, anticholinergics (atropine) or adrenergic agonists (ephedrine) are utilized, while tachycardia may require beta-blockers or calcium channel blockers, cautiously administered․
Inotrope support, like dobutamine, enhances contractility in cases of myocardial dysfunction․ Antiarrhythmics (amiodarone, lidocaine) manage arrhythmias, guided by ECG monitoring․
Vasopressors and vasodilators fine-tune blood pressure, always considering individual patient factors and surgical demands․
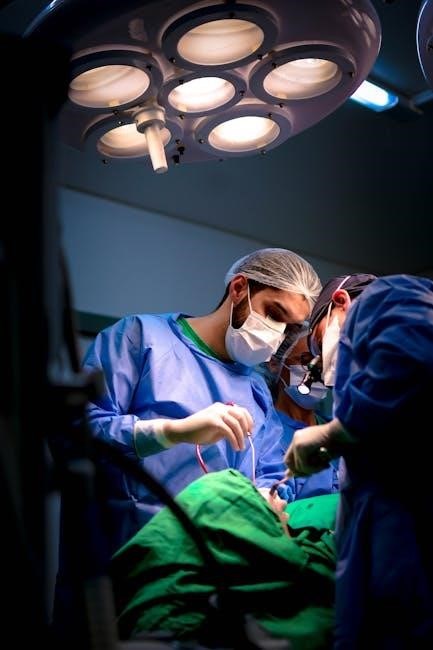
Specific Surgical Procedures ⎼ Anesthetic Management
Anesthesiologists Manual of Surgical Procedures details tailored anesthetic approaches for diverse surgeries, including neurosurgery, obstetrics, pediatrics, orthopedics, and cardiac/thoracic cases․
Neuroanesthesia: Functional Neurosurgery Considerations
Functional neurosurgery, encompassing procedures like deep brain stimulation (DBS) for movement disorders and epilepsy, demands meticulous anesthetic management․ Anesthesiologists Manual of Surgical Procedures emphasizes maintaining stable hemodynamics and avoiding fluctuations in cerebral blood flow․
Stereotactic techniques and MR-guided focused ultrasound require precise patient positioning and intraoperative monitoring․ Neuromonitoring, including somatosensory evoked potentials (SSEPs) and motor evoked potentials (MEPs), is crucial for safeguarding neurological function during these delicate procedures․ Careful titration of anesthetic agents is essential to facilitate accurate neurological assessment․
Obstetric Anesthesia: Labor and Cesarean Section
Anesthesiologists Manual of Surgical Procedures details comprehensive obstetric anesthesia techniques for both labor and cesarean sections․ Managing labor analgesia, including epidural and spinal anesthesia, requires careful titration to provide effective pain relief while preserving maternal motor function;
Cesarean section anesthesia necessitates rapid sequence induction and intubation to ensure a secure airway and prevent aspiration․ Hemodynamic stability is paramount, given the physiological changes of pregnancy․ Postoperative pain management protocols are also crucial for maternal comfort and recovery․
Pediatric Anesthesia: Age-Specific Challenges
Anesthesiologists Manual of Surgical Procedures emphasizes the unique considerations in pediatric anesthesia, acknowledging significant age-related physiological differences․ Securing airway access in infants and children demands specialized equipment and techniques, differing from adult approaches․
Maintaining normothermia is critical due to increased surface area-to-mass ratio․ Drug dosing must be carefully calculated based on weight, and monitoring requires age-appropriate sensors․ Addressing parental anxiety and providing a child-friendly environment are also essential components of care․
Orthopedic Anesthesia: Regional Techniques and Positioning
Anesthesiologists Manual of Surgical Procedures highlights the frequent use of regional anesthesia in orthopedic cases, including nerve blocks for upper and lower extremities, minimizing systemic effects․ Careful patient positioning is paramount to prevent nerve injury and circulatory compromise during lengthy procedures․
Considerations include padding pressure points, avoiding excessive traction, and monitoring for signs of compartment syndrome․ Intravenous analgesia and multimodal pain management strategies are crucial for postoperative pain control, optimizing patient recovery․
Cardiac and Thoracic Anesthesia: One-Lung Ventilation
Anesthesiologists Manual of Surgical Procedures details the complexities of one-lung ventilation (OLV) for thoracic surgery, emphasizing meticulous airway management and ventilation strategies․ Maintaining adequate oxygenation and minimizing hypoxemia in the non-ventilated lung are critical․
Careful monitoring of hemodynamics, including pulmonary artery catheterization when indicated, is essential․ Bronchoscopic guidance confirms proper endotracheal tube placement, while addressing potential complications like airway edema or bleeding․
Minimally Invasive Procedures: Anesthetic Adaptations
Anesthesiologists Manual of Surgical Procedures highlights anesthetic adaptations for minimally invasive surgery, focusing on considerations like pneumoperitoneum’s physiological effects․ CO2 insufflation impacts venous return and cardiac output, requiring careful fluid management and hemodynamic support․
Regional anesthesia techniques are often favored, alongside multimodal analgesia to minimize opioid consumption․ Maintaining precise control of ventilation and addressing potential for steep Trendelenburg positioning are crucial for patient safety and optimal surgical outcomes․
Pain Management
Anesthesiologists Manual of Surgical Procedures details neuraxial analgesia, multimodal protocols, and postoperative strategies for effective pain control, enhancing patient recovery․
Neuraxial Analgesia: Principles and Techniques
Neuraxial analgesia, as outlined in Anesthesiologists Manual of Surgical Procedures, involves techniques like epidural and spinal anesthesia for targeted pain relief․
The manual emphasizes establishing departmental policies and procedures for safe and effective neuraxial administration․
It highlights the importance of interdepartmental collaboration – including nursing, pharmacy, and surgery – to optimize patient outcomes․
Proper technique selection, dosage, and monitoring are crucial, alongside diligent management of potential complications․
Multimodal Analgesia Protocols
Anesthesiologists Manual of Surgical Procedures advocates for multimodal analgesia, combining various techniques to minimize opioid reliance and enhance pain control․
Protocols integrate preemptive analgesia, local anesthetics, NSAIDs, and adjuvant medications for synergistic effects․
The manual stresses the importance of individualized plans, considering surgical factors and patient characteristics․
Acute Pain Services, as detailed, play a vital role in developing and implementing these protocols, fostering interdepartmental collaboration for optimal postoperative pain management․
Postoperative Pain Control Strategies
Anesthesiologists Manual of Surgical Procedures emphasizes a proactive approach to postoperative pain control, extending beyond the operating room․
Strategies include neuraxial techniques, oral analgesics, and regional anesthesia, tailored to the surgical procedure and patient needs․
The manual highlights the Acute Pain Service’s role in implementing protocols and monitoring patient outcomes, ensuring effective pain management․
Minimizing opioid consumption and addressing potential complications like PONV are central to these comprehensive strategies․
Anesthetic Pharmacology
Anesthetic pharmacology, as detailed in the manual, covers inhalation and intravenous agents, alongside neuromuscular blockers—focusing on selection, dosage, monitoring, and reversal techniques․
Inhalation Anesthetics: Mechanisms and Effects
Inhalation anesthetics, crucial components of anesthetic practice, exert their effects through complex mechanisms impacting the central nervous system․ The Anesthesiologists Manual of Surgical Procedures details how these agents modulate neuronal activity, leading to both analgesia and unconsciousness․
Understanding their specific effects on cardiovascular and respiratory systems is paramount․ The manual emphasizes the importance of considering factors like Minimum Alveolar Concentration (MAC) and solubility when selecting and administering these potent drugs, ensuring patient safety and optimized anesthetic management throughout surgical interventions․
Intravenous Anesthetics: Selection and Dosage
Intravenous anesthetics offer rapid induction and precise control, vital for surgical anesthesia, as detailed in the Anesthesiologists Manual of Surgical Procedures․ Careful agent selection—propofol, etomidate, ketamine, and others—depends on patient factors and surgical needs․
Dosage adjustments are critical, guided by hemodynamic stability and desired depth of anesthesia․ The manual stresses individualized titration, considering age, weight, and comorbidities, to minimize adverse effects and ensure optimal patient outcomes during the entire perioperative period․
Neuromuscular Blocking Agents: Monitoring and Reversal
Neuromuscular blocking agents (NMBAs) facilitate surgical conditions, but require vigilant monitoring, as outlined in the Anesthesiologists Manual of Surgical Procedures․ Objective monitoring—train-of-four (TOF) or double-burst stimulation—is essential to assess blockade depth and guide dosage adjustments․
Reversal agents, like neostigmine and sugammadex, restore neuromuscular function․ The manual emphasizes timely reversal to prevent postoperative respiratory complications, ensuring patient safety and a smooth emergence from anesthesia․
Complications and Their Management
The manual details prompt recognition and treatment of critical events like anaphylaxis and malignant hyperthermia, alongside PONV prophylaxis strategies for patient safety․
Anaphylaxis: Recognition and Treatment
Anesthesiologists Manual of Surgical Procedures emphasizes rapid identification of anaphylactic reactions, characterized by hypotension, bronchospasm, and urticaria․ Immediate cessation of triggering agents is crucial․
Treatment protocols involve epinephrine administration as the primary intervention, alongside volume resuscitation with intravenous fluids and airway management, potentially requiring intubation․
Vasopressors may be necessary to maintain hemodynamic stability, while antihistamines and corticosteroids provide adjunctive support, mitigating further inflammatory responses and ensuring patient well-being․
Malignant Hyperthermia: Prevention and Management
Anesthesiologists Manual of Surgical Procedures highlights preemptive risk assessment for malignant hyperthermia (MH), particularly in susceptible patients undergoing volatile anesthetic exposure․
Early recognition involves monitoring for unexplained tachycardia, masseter spasm, and rapidly rising end-tidal CO2․ Immediate dantrolene administration is paramount, interrupting calcium release within muscle cells․
Supportive care includes active cooling, alkalization with bicarbonate, and management of hyperkalemia, ensuring vigilant monitoring and prompt intervention to mitigate potentially fatal complications․
Postoperative Nausea and Vomiting (PONV): Prophylaxis
Anesthesiologists Manual of Surgical Procedures emphasizes a multimodal approach to PONV prophylaxis, tailoring strategies to individual patient risk factors․
Combining antiemetics with differing mechanisms—like 5-HT3 receptor antagonists, neurokinin-1 receptor antagonists, and dexamethasone—enhances efficacy․
Minimizing opioid use, employing regional anesthesia when feasible, and ensuring adequate hydration are crucial preventative measures, improving patient comfort and recovery postoperatively․
Equipment and Technology
Anesthesiologists Manual of Surgical Procedures details anesthesia machine function, monitoring device interpretation, and troubleshooting, alongside advancements shaping modern anesthetic practice․
Anesthesia Machine: Function and Maintenance
The anesthesia machine is a complex system delivering gases, monitoring parameters, and supporting ventilation․ Anesthesiologists Manual of Surgical Procedures emphasizes understanding its components – vaporizers, flowmeters, and scavenging systems – for safe operation․
Regular maintenance, including leak checks, calibration of flowmeters, and vaporizer inspections, is crucial․ Proper function ensures accurate gas delivery and patient safety․ Routine preventative maintenance schedules, detailed in the manual, minimize downtime and potential hazards during critical surgical moments․
Monitoring Devices: Interpretation and Troubleshooting
Anesthesiologists Manual of Surgical Procedures highlights the critical role of monitoring devices – ECG, pulse oximetry, capnography, and invasive pressure monitoring – in guiding anesthetic management․ Accurate interpretation of waveforms and numerical values is paramount for timely intervention․
The manual details common troubleshooting steps for alarms and inaccurate readings․ Understanding potential causes, like electrode displacement or sampling line kinks, ensures reliable data․ Proficiency in device operation and problem-solving directly impacts patient safety and optimal outcomes․
Advanced Technologies in Anesthesia
Anesthesiologists Manual of Surgical Procedures acknowledges the evolving landscape of anesthesia, incorporating discussions on advanced technologies․ This includes topics like artificial intelligence (AI) applications for predictive analytics and personalized drug delivery systems․
The manual explores the integration of machine learning algorithms to optimize ventilation strategies and enhance hemodynamic stability․ Furthermore, it addresses the potential of robotic assistance in regional anesthesia and the implications of these innovations for improved patient care and workflow efficiency․
Acute Pain Service & Interdepartmental Collaboration
Anesthesiologists Manual of Surgical Procedures emphasizes establishing an acute pain service, fostering collaboration with nursing, pharmacy, surgery, and materials management departments․
Establishing an Acute Pain Service
Anesthesiologists Manual of Surgical Procedures highlights the critical need for each anesthesia department to proactively establish a dedicated acute pain service․ This service assumes responsibility for developing and implementing comprehensive policies and procedures specifically focused on neuraxial analgesia techniques․
Successful implementation necessitates actively seeking participation from various allied departments, including nursing staff, pharmacy professionals, surgical teams, and materials management personnel, ensuring a truly multidisciplinary approach to postoperative pain control and enhanced patient outcomes․
Liaison with Surgical Departments
Anesthesiologists Manual of Surgical Procedures emphasizes the importance of fostering strong collaborative relationships between the anesthesia and surgical departments․ Effective communication and coordination are paramount for optimizing patient care throughout the perioperative period․
This liaison facilitates a shared understanding of surgical approaches, anticipated physiological challenges, and individualized anesthetic plans, ultimately contributing to improved surgical outcomes and enhanced patient safety through proactive planning and seamless teamwork․
Policies and Procedures for Neuraxial Analgesia
Anesthesiologists Manual of Surgical Procedures highlights the necessity of establishing clear, comprehensive policies and procedures governing neuraxial analgesia within the anesthesia department․ These protocols should encompass patient selection criteria, technique standardization, and diligent post-operative monitoring․
Detailed guidelines are crucial for minimizing risks, ensuring consistent quality of care, and promoting safe, effective pain management utilizing neuraxial techniques, aligning with best practices and institutional standards․
Future Trends in Surgical Anesthesia
Anesthesiologists Manual of Surgical Procedures anticipates advancements like artificial intelligence and personalized anesthesia, revolutionizing patient care and optimizing anesthetic approaches․
Artificial Intelligence in Anesthesia
Artificial intelligence (AI) is poised to transform anesthesia, as highlighted within the Anesthesiologists Manual of Surgical Procedures․ AI algorithms can analyze vast datasets to predict patient responses, optimize drug delivery, and enhance hemodynamic stability․
Machine learning models can assist in real-time monitoring, early detection of complications, and personalized anesthesia plans․ This includes predictive modeling for postoperative pain and resource allocation, ultimately improving patient outcomes and streamlining workflows for anesthesiologists․
The manual suggests AI will become integral to future anesthetic practice․
Personalized Anesthesia Approaches
The Anesthesiologists Manual of Surgical Procedures emphasizes a shift towards personalized anesthesia, moving beyond standardized protocols․ This involves tailoring anesthetic plans based on individual patient characteristics, including genetics, physiology, and surgical factors․
Pharmacogenomics will play a crucial role, optimizing drug selection and dosage to minimize adverse effects and maximize efficacy․ Continuous monitoring and data analysis will enable real-time adjustments, ensuring optimal patient comfort and safety throughout the surgical journey․
Precision anesthesia is the future․